|
If you have been diagnosed as having Fatty Liver Disease, you may be wondering if there are treatment options available that can help. Fatty Liver Disease is very common. Following a canine liver disease diet is an important treatment tool for dogs with compromised liver function. A dietary change for a dog with canine liver disease. What is a liver shunt in dogs? A portosystemic shunt (PSS) or liver shunt is a condition where the normal flow of blood, to and through the liver, is markedly reduced. University of Maryland Medical Center. Description. An in- depth report on the causes, diagnosis, treatment, and prevention of cirrhosis. Causes include: Alcoholism. Chronic hepatitis B and CAutoimmune hepatitis. Bile duct disorders such as primary biliary cirrhosis and primary sclerosing cholangitis. Nonalcoholic fatty liver disease (NAFLD), which includes nonalcoholic steatohepatitis (NASH)Metabolic disorders such as hemachromatosis, Wilson’s disease, and alpha- 1 antitrypsin deficiency. Prolonged exposure to certain chemicals and medications. 
Get information on psoriasis causes, treatment, medication, and types: scalp, vulgaris, guttate, inverse, and pustular. Red dry flakes, skin scales, and plaques of. If your dog has a liver shunt or portosystemic shunt you've come to the right place. Liver shunt in dogs can be helped naturally, possibly avoiding traumatic and. Liver Disease: Signs, Symptoms, and Diagnosis. Column written by: Dr. Fleming, Sherwood Animal Clinic (Regina, Saskatchewan, Canada) This topic is as big as the. Cirrhosis is a chronic liver disease that is the result of damage to liver tissue with scarring of the liver (fibrosis - nodular regeneration) causing progressive. Causes of Liver Disease. Liver disease is a broad category of other, more specific, diseases. These specific conditions that cause liver disease can work alone or in. Complications. Cirrhosis can cause many serious complications including: Ascites (fluid buildup in the abdomen)Variceal hemorrhage, severe bleeding from varices (enlarged veins in the esophagus and upper stomach)Spontaneous bacterial peritonitis, a severe infection of the membrane lining of the abdomen. Hepatic encephalopathy, impaired mental function caused by buildup in the body of toxins such as ammonia. Hepatocellular carcinoma, a type of liver cancer. Hepatorenal syndrome, when kidney failure occurs along with severe cirrhosis. Dietary and Lifestyle Changes. All patients with cirrhosis can benefit from certain lifestyle interventions. These include: Stop drinking alcohol. Restrict dietary salt. Follow a good diet plan, which may include protein restriction. 
Get vaccinations for influenza, hepatitis A and B, and pneumococcal pneumonia (if recommended by your doctor). Inform your doctor of all prescription and nonprescription medications, and any herbs and supplements, you take or are considering taking. Treatment. Cirrhosis is an irreversible condition. Treatment focuses on slowing the progression of liver damage and reducing the risk of further complications. Your doctor will treat any underlying medical conditions that are the cause of your cirrhosis. If liver damage progresses to liver failure, patients may be candidates for liver transplantation. Liver donations can come from either a cadaver or from a living donor. 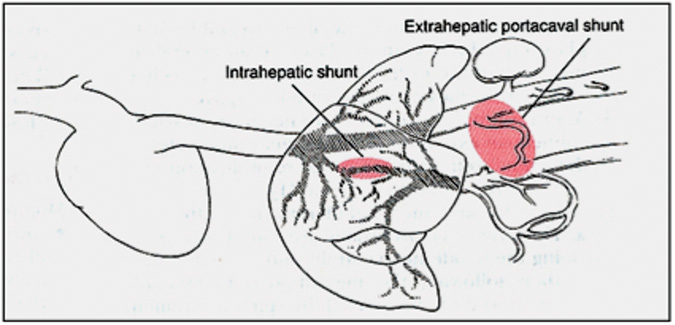
Patients with cirrhosis who have a liver transplant have very good chances for survival. Introduction. Cirrhosis is an irreversible result of various disorders that damage liver cells over time. Eventually, damage becomes so extensive that the normal structure of the liver is distorted and its function is impaired. Cirrhosis is a chronic liver disease that is the result of damage to liver tissue with scarring of the liver (fibrosis - nodular regeneration) causing progressive decrease in liver function, excessive fluid in the abdomen (ascites), bleeding disorders (coagulopathy), increased pressure in the blood vessels (portal hypertension), and brain function disorders (hepatic encephalopathy). Gastritis doesn't always cause signs and symptoms. Nearly everyone has had indigestion and stomach irritation. Most cases of indigestion are.
Excessive alcohol use is the leading cause of cirrhosis. The main damage in cirrhosis is triggered by scarring (fibrosis) that occurs from injuries due to alcohol, viruses, or other assaults. The scar tissue and other changes in liver cells gradually replace healthy liver tissue and act like small dams to alter the flow of blood and bile in and out of the liver. Altered Blood and Bile Flow. The changes in blood and bile flow have significant consequences, with both the liver and other organs responding to the altered flow: The small blood vessels and bile ducts in the liver itself narrow (constrict). Blood vessels in other organs, including the kidney, also narrow. Blood flow coming from the intestine into the liver is slowed by the narrow blood vessels. 
It backs up through the portal vein and seeks other routes. Enlarged, abnormally twisted and swollen veins called varices form in the stomach and lower part of the esophagus to transport the blood diverted from the liver. Bilirubin also builds up in the bloodstream, resulting in jaundice, a yellowish cast in the skin and eyes, as well as dark- colored urine. Fluid buildup in the abdomen (called ascites), and swelling in the legs (edema) are common. Functions of the Liver. The liver is the largest internal organ in the body. 
In the healthy adult, it weighs about 3 pounds. The liver is wedge- shaped, with the top part wider than the bottom. It is located right below the diaphragm and occupies the entire upper right quadrant of the abdomen. The liver performs over 5. Damage to the liver can impair these and many other processes. Among them are the following: Processing Healthful Nutrients. The liver processes all of the nutrients the body requires, including proteins, glucose, vitamins, and fats. Producing Proteins The liver is the body’s “factory” where many important proteins are made. The blood protein albumin is one example that is often underproduced in patients with cirrhosis. Producing Bile. The liver produces bile, a green- colored fluid that helps the body absorb fats and fat- soluble vitamins. Bile contains bilirubin, a yellow- green pigment produced from the breakdown of hemoglobin, the oxygen- carrying component in red blood cells. Bile also contains bile salts, fatty acids, cholesterol, and other substances. Bile travels from the liver to the gallbladder, where it is stored until after a meal. It is then secreted into the intestines where it helps digest fat. Because bile can also travel directly from the liver to the intestines, patients who have had their gallbladders removed can still absorb fat normally. Eliminating Toxins. One of the liver's major functions is to render harmless potentially toxic substances, including alcohol, ammonia, drugs, and harmful by- products of digestion. Structure of the Liver. The vital processes the liver performs rely on well- organized liver architecture. The basic building blocks of the liver are the following structures: Bile ducts. Blood vessels. Working liver tissue (called the parenchyma)Supportive (connective) tissue. The liver is a built on a framework of lobes: Lobes. The liver is divided into two major lobes, a right and a smaller left, which are separated by tough, fibrous connective tissue. Lobules. The liver's two major lobes contain about 1. Each lobule contains microscopic columns of liver cells and blood vessels. Bracing the corners of each lobule column are an artery and a vein that carry blood and a bile duct that drains bile. Bile ducts. The bile ducts in the column corners collect bile draining from tiny canals around the liver cells. These ducts eventually join to form the large common bile duct that leads from the liver to the gallbladder. Arteries and veins. The arteries bring oxygen- rich blood to nourish the liver cells. The veins supply the liver cells with blood containing the nutrients and toxins that the liver cells process. A central vein runs through each column and collects the processed blood from both sources. These veins join to form the hepatic vein. The Liver's Blood Supply. The liver is rich in blood. Its vessels contain about a pint, or 1. It gets its blood from two large vessels, the hepatic artery and the portal vein, and is drained of blood by the hepatic vein. This artery carries blood from the heart directly to the liver. This blood nourishes the liver. The portal vein. The portal vein carries blood that has circulated through the stomach, spleen, and intestine to the liver. The liver processes this blood, extracting nutrients and toxins. The hepatic vein. This vein carries blood away from the liver and connects to the inferior vena cava, a large vein that carries blood back to the heart. Alcoholic liver disease includes fatty liver (build- up of fat cells in the liver), alcoholic hepatitis (inflammation of the liver caused by heavy drinking), and alcoholic cirrhosis. Alcoholic cirrhosis is the primary type of cirrhosis in the U. S. It develops in 1. People who drink heavily and who also have hepatitis C are at particular risk of developing cirrhosis. In the liver, alcohol converts to toxic chemicals that trigger inflammation and tissue injury, which lead to cirrhosis. Chronic Viral Hepatitis. Chronic viral hepatitis, both hepatitis B and hepatitis C, is another primary cause of cirrhosis. Chronic hepatitis C is a more common cause of cirrhosis in developed countries, while hepatitis B is a more common cause of cirrhosis worldwide, especially in sub- Saharan Africa and parts of Asia. People with chronic hepatitis B who are co- infected with hepatitis D are especially at risk for cirrhosis. The longer a patient has had chronic hepatitis, the greater the risk for eventually developing cirrhosis. Hepatitis viruses can produce inflammation in liver cells, causing injury or destruction. If the condition is severe enough, the cell damage becomes progressive, leading to scar tissue in the liver. In advanced cases, the liver shrivels in size, a condition called postnecrotic or posthepatic cirrhosis. Hepatitis C is a virus- caused liver inflammation which may lead to jaundice, fever, and cirrhosis. The people most at risk for contracting and spreading hepatitis C are those who share needles for injecting drugs and health care workers or emergency workers who may be exposed to contaminated blood. People who have autoimmune hepatitis also often have other autoimmune conditions, including systemic lupus erythematosus, rheumatoid arthritis, Sj. Autoimmune hepatitis typically occurs in women ages 1. Bile Ducts Disorders. Disorders that block or damage the bile ducts can cause bile to back up in the liver, leading to inflammation and cirrhosis. These diseases include primary biliary cirrhosis and primary sclerosing chlorangitis. Primary Biliary Cirrhosis. Up to 9. 5% of primary biliary cirrhosis (PBC) cases occur in women, usually around age 5. In people with PBC, the immune system attacks and destroys cells in the liver’s bile ducts. Like many autoimmune disorders, the causes of PBC are unknown. Primary Sclerosing Cholangitis. Primary sclerosing cholangitis (PSC) is a chronic disease that mostly affects men, usually around age 4. The cause is unknown, but immune system defects, genetics, and infections may play a role.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
June 2017
Categories |
 RSS Feed
RSS Feed
